|

Custom Search
|
|
Dermpath-India Pathology of Lipoblastoma 2022 |
|
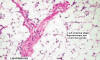
Lipoblastoma is a rare
benign mesenchymal tumour of embryonal fat that occurs almost exclusively
in infants and children.
The term lipoblastoma was first used by Jaffe (Recurrent lipomatous tumors of the groin: liposarcoma and lipoma pseudomixomatodes. Arch Pathol 1926;1:381–387). Vellios et al used the term 'Lipoblastomatosis' for an infiltrating lipoblastoma in the supra-clavicular region, anterior chest wall, and axilla (Lipoblastomatosis: a tumor of fetal fat different from hibernoma: report of a case, with observations on the embryogenesis of human adipose tissue. Am J Pathol 1958;34:1149–1159). Age: Usually occurs in infants and young children (between 5 days to 6 years). Maturing lipoblastomas may be present in older children and rarely in teenagers. These may take the appearance of fibrolipoma. Site: Most commonly found in the subcutis of the upper and lower extremities. Lipoblastomas are also located in less common sites, including head and neck, mediastinum, lung, trunk, mesentery, peritoneal cavity, retroperitoneum, intramuscular, and inguinal canal. Clinical presentation: Lipoblastoma presents as a painless nodule or mass. The disease is presents in two forms: I- Superficial- (embryonal or fetal lipoma)-Solitary subcutaneous circumscribed slow growing lesion. II- Diffuse - (Lipoblastomatosis) - Multicentric, deep-seated and ill-defined, diffuse lesion which arises in skeletal muscle, retroperitoneum, or mesentry. Lipoblastomatosis may occur in association with hemangiomas, other soft tissue lesions, intestinal neuronal dysplasia and/or macrodactyly. Gross: The tumour presents as lobulated, soft, and encapsulated mass with a tan yellow to creamy white cut surface. The lesion is paler than an ordinary lipoma, with mottled gray myxoid areas. Microscopic features: Lipoblastomas is subclassified into the following 4 subtypes, according to their histological features: (1) the classic type, characterized by a minimal myxoid component consisting of intercellular mucin, spindle cells, and stellate primitive mesenchymal cells together with adipocytic component; (2) myxoid lipoblastomas contained abundant interstitial mucin, which comprised more than 50% of the specimen. (3) lipoma-like lipoblastomas lacked a myxoid component and are composed predominantly of mature adipocytes with scattered monovacuolated and multivacuolated lipoblasts; and (4) hibernoma-like lipoblastomas lacked a myxoid component and are composed predominantly of multivacuolated lipoblasts, some of which had central nuclei and granular eosinophilic cytoplasms. Summary of microscopic features: Lobulated tumour composed of mature and immature adipocytes. Immature fat cells resemble embryonic white fat. A mixture of lipoblasts in different stages of maturation- from univacuolated spindle mesenchymal cells within the myxoid matrix to larger and more vacuolated cells to the mature adipocytes may be present. There are large cells with granular cytoplasm resembling hibernoma cells. There are no atypical mitotic figures and no nuclear atypia. The cells are present in a stroma which is often myxoid with a rich delicate plexiform vascular network. Cytogenetics: Shows rearrangements of chromosome 8 Differential diagnosis: Confusion with myxoid liposarcoma, well-differentiated liposarcoma and typical lipomas may occur. Myxoid liposarcoma is rare under the age of 10 years. In lipoblastoma there is prominent lobulation, with maturation at the center of the lobules. In myxoid liposarcoma, maturation is at the periphery. Cytologic features suggestive of malignant potential, such as nuclear atypia, mitotic figures, hyperchromasia, and hypercellularity, are relatively uncommon in lipoblastoma. Lipoblastomas have been reported to exhibit karyotypic abnormalities involving chromosome 8, while lacking the translocation associated with myxoid liposarcoma. Treatment : Depending on the size and location the tumour may compress adjacent structures and interfere with their functions. Complete excision is the treatment of choice. The diffuse form can be difficult to excise completely which may lead to recurrence of the tumour. A followup of at least two years is suggested.
|
|
|