|

Custom Search
|
|
Infectious Disease Online Pathology of Rhinosporidiosis Dr Sampurna Roy MD 2022
|
 |

|
Rhinosporidiosis is a granulomatous infection of mucocutaneous tissue
caused by Rhinosporidium seeberi. It was first described by Guillermo Seeber in Buenos Aires, Argentina. Rhinosporidium seeberi is an aquatic protozoan and recent taxonomy suggests it is in a new eukaryotic group of protists known as Mesomycetozoa. Hot tropical climates have been found to be the most suitable environment for this organism.
The disease is endemic in India and Sri Lanka, but sporadic cases has also
been reported from United States, South America and Iran.
The lesion produces reddish polypoidal, bulky, friable mucosal masses in the nasal cavity and nasopharynx. Less frequently the infection involves the conjunctiva, mouth, larynx, genitalia and skin. The infection results from a local traumatic inoculation with the organism while swimming or bathing in freshwater ponds, lakes or rivers. Nasal rhinosporidiosis- The patient complains of swelling and foreign body sensation in the nose accompanied by itching, sneezing and bleeding. Initially the lesions are small and sessile but they progress to large and pedunculated 'strawberry-like' polypoid mass. The patients may also complain of dysphagia and dyspnea when lesions high in the turbinates protrude from the nares or into the nasopharynx. Ocular rhinosporidiosis- The lesions involve the palpebral conjunctiva. Early lesons are asymptomatic but eventually cause discharge, photophobia, redness and secondary infection. Cutaneous rhinosporidiosis-
The skin lesions begin as
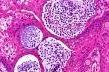
papillomas which become warty and exude myxomatous material. Histopathological features: There is granulation tissue containing plasma cells, lymphocytes, focal collection of histiocytes and neutrophils. The overlying epithelium is hyperplastic with focal thinning and occasional ulceration. Rhinosporidium seeberi has a distinctive morphology in the tissue section. The sporangia are located predominantly in the stroma of the mucosal polyp. The largest sporangia are usually in a subepithelial location. The size of the globular sporangia depend on the stage of maturation. Young trophic forms (immature sporangia) are spherical,10-100 micrometer in diameter and have a central basophilic nucleus. These develop into mature sporangia by a process of progressive enlargement and endosporulation. Mature sporangia are 100 to 350 micrometer in diameter, have a thick chitinous wall and contain spores in different stages of development. The spores are 8-10 micrometer in diameter and contain globular eosinophilic inclusions. Spores are released through a pore or by rupture of the wall at the site of the pore. The ruptured sporangia may elicit a foreign body reaction. The released spores incite a neutrophilic response in the tissue. These spores are also passed in the nasal discharge. The spores in the tissue develop into small trophic forms thus enlarging the lesion. Special stains: Rhinosporidium Seeberi is visualized by fungal stains such as PAS, Gomori's methenimine silver and mucicarmine. The lesion is treated by surgical excision. Recurrence is common and may require repeated excisions over a period of many years.
|
|
|
 |