|

Custom Search
|
|
Infectious Disease Online Pathology of Rhinoscleroma Dr Sampurna Roy MD 2022
|
 |
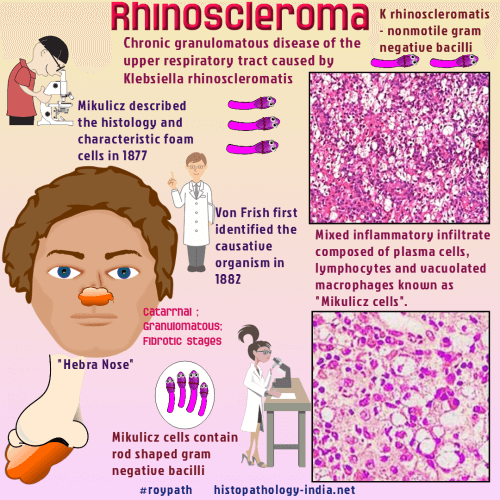
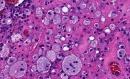
Rhinoscleroma is a chronic granulomatous disease of the nasal mucosa (less commonly, nasopharynx, larynx, and trachea) caused by Klebsiella rhinoscleromatis, an encapsuted, nonsporulating, nonmotile gram-negative bacillus.Rhinoscleroma is prevalent in the USSR, Poland, and central Europe and is endemic in Mexico, Central America, and upper South America. Age and sex: Rhinoscleroma is a disease of young and middle-aged adults, slightly more common in women and without racial predisposition. Clinical presentation: The onset is slow and insidious, usually over many years, and the patient’s general health is unaffected. At first, the symptoms are those of a common cold. An initial granularity of the nasal mucosa is replaced by reddish, waxy, granulomatous infiltrates and firm, nodular, intranasal masses. In fully developed rhinoscleroma hyperplastic changes of the alae and tip of the nose (the "Hebra nose") are severely disfiguring. Airway obstruction, anaemia, and speech difficulties develop as the disease advances. Anesthesia of the soft palate and enlargement of the uvula suggest rhinoscleroma, but any part of the upper airways, the paranasal sinuses and orbit may be involved. Compressive destruction of bone and soft tissue mimics invasive tumours. Scar tissue persists after the disease runs its course. Pathological features: There are 3 pathologic stages of development. (i) the catarrhal stage, ii) granulomatous stage, iii) and fibrotic stage. In the catarrhal stage, the mucosa consists of inflamed granulation tissue containing neutrophils and cellular debris. In the granulomatous stage, the characteristic lesion of rhinoscleroma is seen. In the fibrotic stage, the characteristic Mikulicz cells are absent, fibrosis is extensive, and the inflammatory infiltrate contains lymphocytes and plasma cells.
Differential diagnosis: Granulomatous bacterial, fungal, or protozoan infections ; vasculitis ; and tumours involving the nose and upper airways, including the lips and soft palate. Rhinoscleroma should be distinguished from tuberculosis , leprosy , syphilitic gumma , histoplasmosis , blastomycosis, paracoccidioidomycosis , rhinosporidiosis , leishmaniasis , Wegener granulomatosis , T-cell/natural killer cell lymphomas , and carcinomas. Diagnosis of Rhinoscleroma: The diagnosis of rhinoscleroma is confirmed by isolating Klebsiella rhinoscleromatis in culture or by demonstrating the organism in tissue sections. The bacteria stain very well with periodic acid-Schiff, Giemsa, Gram, and silver stains. Pathogenesis: The pathogenesis of rhinoscleroma is not clear. Cellular immunity is impaired in these patients. Humoral immunity is preserved. The CD4-CD8 ratio within the lesion is altered, showing decreased CD4 lymphocytes and increased CD8 lymphocytes, possibly inducing a diminished T-cell response. The macrophages are not fully activated (hence groups of histiocytes instead of bactericidal epithelioid macrophages are seen in the granulomatous stage). Rhinoscleroma in patients with human immunodeficiency virus infection has also been reported. The mucopolysaccharides of the bacterial capsule probably contribute to inhibition of phagocytosis. Treatment: Antibiotic of choice are streptomycin, tetracycline, and chloramphenicol. In some patients surgical intervention is necessary to relieve airway obstruction or to repair the facial features.
|