|

Custom Search
|
|
Dermpath-India Pathology of Schwannoma Dr Sampurna Roy MD 2022
|
 |
|
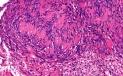
Syn: Neurilemmoma Visit: Pathology of Epithelioid Schwannoma Schwannomas (Neurilemmoma) are slow growing benign nerve sheath tumours. These are usually solitary lesions. Multiple lesions are rare and may occur in the following clinical settings: i) multiple localized tumours. ii) In association with neurofibroma in von Recklinghausen's disease. iii) In schwannomatosis, a non hereditary disease characterized by multiple subcutaneous and intradermal schwannomas together with tumours of internal organs. Age: Common in patients between the ages of 20 and 50. Site: These are usually located on the head and neck and flexor surface of upper and lower extremities. The spinal roots, cervical, sympathetic, vagus and ulnar nerves are commonly involved. The deeply located lesions are situated in the retroperitoneum and the posterior mediastinum. Gross: The tumour is surrounded by true capsule consisting of the epineurium. Tumour arising in a small nerve resemble a neurofibroma and often obliterate the nerve of origin. Tumours arising in larger nerves present as eccentric masses. Cut surface reveals smooth, glistening, grey-white appearance. There may be cystic areas with areas of hemorrhage and calcification.
Immunohistochemistry: S100 protein is strongly expressed by most cells of schwannoma. The cells also express Vimentin and myelin basic protein. Differential diagnosis: Neurofibroma ; Palisaded encapsulated neuroma (more number of axons and Schwann cells in interlacing fascicles together with cleft like spaces. Cutaneous leiomyoma (smooth muscle actin and desmin positive) ; Palisaded myofibroblastoma ( involve lymph nodes, contain fibroblastic and myofibroblastic cells and are S100 protein negative).
Cellular Schwannoma This variant is usually found in the deeper tissues (retroperitoneum or mediastinum).
Differential diagnosis include low grade malignant peripheral nerve seath tumour and leiomyosarcoma. Immunohistochemistry reveals strong and diffuse positivity with S100 protein. Desmin is negative. Further reading: Cellular schwannoma. A clinicopathologic, DNA flow cytometric, and proliferation marker study of 70 patients. Cellular schwannoma: a distinct pseudosarcomatous entity.
Melanotic Schwannoma This rare variant usually occurs in middle aged adults and commonly arises from the posterior spinal nerve roots. Melanotic schwannomas are well circumscribed, partly encapsulated lesions characterized by polygonal and vesicular cells with grooved nuclei. These cells contain abundant melanin pigment. In psammomatous melanotic schwannoma, varying numbers of psammoma bodies are present. Some of these cases are associated with Carney's complex (myxoma, spotty pigmentation and endocrinopathy). Malignant melanotic schwannoma usually arises from the sympathetic chain and is characterized by brisk mitosis and prominent nucleoli. Immunohistochemistry reveals that tumour cells stain positively for S100 protein, HMB45, MART-1, synaptophysin and vimentin.
Neuroblastoma - like Schwannoma
Benign schwannomas may contain rosette-like
structures mimicking neuroblastoma/PNET.
Tumour cells are positive for S100 protein and negative for neuronal
markers synaptophysins and neurofilament protein.
MIC2 is negative (rules out PNET type
differentiation).
Individual cells were surrounded by type IV collagen.
This is a feature characteristically seen in schwannian but not in
neuronal tumours. Further
reading:
Neuroblastoma-like
neurilemoma.
Schwannoma
with Neuroblastoma-Like Rosettes: An Unusual Morphologic Variant.
Neuroblastoma-like schwannoma: a case report and review of the
literature.
Plexiform Schwannoma
Plexiform schwannoma may demonstrate conventional, cellular, or mixed appearance. Site: 1) Common superficial (dermal and subcutaneous) tumours. 2) Deep somatic soft tissue. Worrying histologic features are increased cellularity and mitoses. Differential diagnosis: Plexiform neurofibromas and malignant peripheral nerve sheath tumour. Further reading: Congenital and childhood plexiform (multinodular) cellular schwannoma: a troublesome mimic of malignant peripheral nerve sheath tumor. Plexiform schwannoma of the small intestine: report of a case.
|
|
Glandular Schwannoma: This is a rare subtype of schwannoma. The tumours are usually small and superficial. Microscopic examination shows that the tumour is composed of a spindle cell component and glandular structures. The spindle cell component stain positively for S-100 protein. The glandular epithelium stain with CAM 5.2 and epithelial membrane antigen but not with S-100 protein. This variant can be distinguished from the pseudoglandular schwannoma by immunohistochemical staining. Further reading: Benign glandular schwannoma and Recklinghausen disease. Report of a case.
Benign glandular
schwannoma. Pseudoglandular Schwannoma: Pseudoglandular schwannoma is an unusual variant of benign schwannoma. It is characterized by the presence of glandlike structures lined with Schwann cells. The pathological findings are consistent with a pseudoglandular schwannoma composed of typical Schwann cells arranged in an Antoni B pattern, with numerous large pseudocystic spaces. Immunohistochemical examination of the sections reveal that the cells lining the pseudoglandular spaces are not only diffusely reactive for S100 protein, but also demonstrate focal positivity for epithelial membrane antigen and cytokeratins AE and AE3. Further reading: Cutaneous Cellular Pseudoglandular Schwannoma: An Unusual Histopathologic Variant. Schwannomas with pseudoglandular elements: clinicopathologic study of 61 cases. Pseudoglandular schwannoma of the cauda equina. Case report. Cutaneous pseudoglandular schwannoma: a case report of an unusual histopathologic variant.
|
Hybrid Peripheral Nerve sheath Tumor (PNST): Hybrid peripheral nerve sheath tumours are distinct entities of PNST. Hybrid PNSTs include hybrid schwannoma-neurofibromas, hybrid schwannoma-perineuriomas and hybrid neurofibroma-perineuriomas. These hybrid tumours usually arise in the dermis and subcutis, and they occur over a wide range of age and anatomical distribution. Further reading: A soft tissue perineurioma and a hybrid tumor of perineurioma and schwannoma. Hybrid Epithelioid Schwannoma/Perineurioma. Nerve sheath tumours with hybrid features of neurofibroma and schwannoma: a conceptual challenge.
|
|
|
 |
Copyright © 2002-2022 histopathology-india.net