|

Custom Search
|
|
Infectious Disease Online Pathology of Babesiosis (Piroplasmosis)
|
|
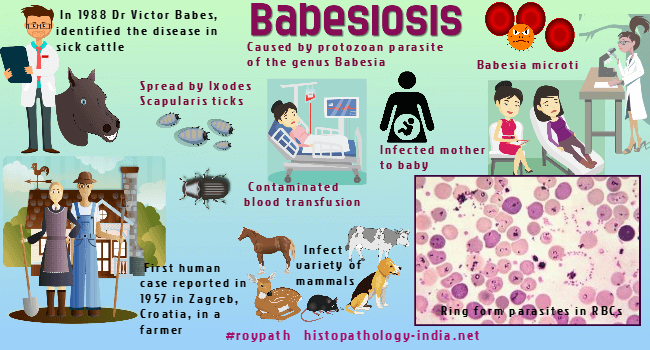
Babesiosis, an infection by protozoan parasite of the genus Babesia, is transmitted by hard-bodied Ixodes scapularis ticks (commonly called blacklegged ticks or deer ticks). In 1888 Dr.Victor Babes, a Romanian pathologist, identified the disease in cattle that had fever and blood stained urine. The first human case was described by Skaraballo in 1957, near Zagreb, Croatia. "A young farmer had been grazing cattle on tick-infested pastures and presented with fever, anemia and hemoglobinuria. He was asplenic and died of renal insufficiency during the second week of illness." Human Babesiosis. Infectious Disease Clinics of North America, 22(3), 469–ix. Babesia microti and Babesia divergens have been identified in most human cases. Although common in animals, babesiosis is rare in humans.
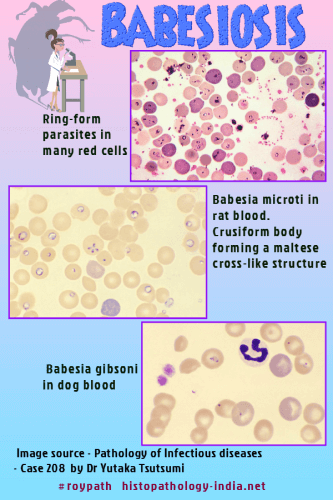
The parasites are intraerythrocytic and are commonly called piroplasms due to the pear-shaped forms found within infected red blood cells. The diagnostic hallmark of babesiosis is the cruciform body (tetrad) forming a maltese cross-like structure. The organisms are transmitted by ixodid ticks and are capable of infecting a wide variety of vertebrate hosts which are competent in maintaining the transmission cycle. The parasites resembling those of malaria, invade and destroy erythrocytes, but differs from malaria parasites in several important ways. They are transmitted by ticks, make no pigment, produce no sexual forms, and have no exoerythrocytic stage. Babesia infect a variety of mammals including cattle, white-footed mouse and white-tailed deer, horses, and dogs. The parasites are ingested by ticks when they feed on infected mammals, multiply in the intestinal epithelium of the ticks, and spread through the insect bodies. The infective organisms are then transmitted in the saliva when the tick feeds again. In Europe, most reported cases are due to Babesia divergens and occur in splenectomized patients. In the United States, Babesia microti is the agent most frequently identified (Northeast and Midwest), and can occur in non-splenectomized individuals. Two variants, have been reported in the U.S. states of Washington and California (WA1- type and related parasites) and Missouri (MO1). After inoculation by the tick, Babesia invade erythrocytes, where they appear as ameboid, round, rod-shaped or irregularly shaped organisms. They are 1 to 5 micrometer in diameter, and with the Giemsa stain have a blue cytoplasm and a mass of red chromatin. Splenectomy and diabetes are predisposing factors. The incubation period varies from 2 to 6 weeks and is followed by sudden onset of chills and fever, sometimes with muscle aches and pains, prostration, jaundice, dark urine, diarrhea, and vomiting. The progressive invasion and destruction of red blood cells causes hemoglobinemia, hemoglobinuria, jaundice, and renal failure. The disease is usually self-limited, but uncontrolled infections can be fatal.
Babesia microti has recently been determined to be the most common transfusion-transmitted pathogen in the United States. Patients who acquire Transfusion-transmitted babesiosis often experience severe illness with an associated mortality rate of about 20%. Autopsies have found parasites in erythrocytes concentrated in congested capillaries of many organs, and especially in the hepatic sinusoids. The diagnosis is made by identifying Babesia in thin blood films. Parasitized erythrocytes may also be identified in tissue specimens.
|
|
|
Copyright © 2022 histopathology-india.net