|

Custom Search
|
|
Dermpath-India Pathology of Intramuscular Myxoma Dr Sampurna Roy MD 2022
|
 |
Intramuscular myxoma is a relatively uncommon benign tumour that presents as a slow growing deeply seated mass confined to the skeletal muscle.
Local surgical excision is almost always curative and recurrence is
extremely rare even in incompletely excised lesions. It is commonly located in the large muscles of the thigh, shoulder, buttocks and rarely upper arm. Although most cases are solitary, multiple lesions have been reported in 5% of patients. Multiple intramuscular myxomas are rare and are usually associated with monostotic or polyostotic fibrous dysplasia and is known as Mazabraud's syndrome.
In some patients intramuscular myxomas are associated with
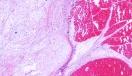
Albright's syndrome. Macroscopically the tumour is well circumscribed, lobulated and gelatinous in appearance. In some cases small fluid filled spaces may be present. Most cases measure between 5 to 10 cms in greatest diameter, but sometimes the tumour may be as large as 20 cms. Histologically the tumour is composed of bland spindle or stellate-shaped cells and abundant myxoid matrix. Some small cells have hyperchromatic nuclei and scanty cytoplasm. In many cases there is almost complete absence of vascular structures in the hypocellular areas. The mucoid material in the backround stroma stains positively with alcian blue and mucicarmine. Some loose collagen bundles may be present. At the periphery the tumour merges with the surrounding muscle. The surrounding muscle fibres may be edematous and atrophic. Cellular myxoma (low-grade myxoid tumour with recurrent potential). This lesion has features in between intramuscular myxoma and low-grade myxofibrosarcoma. There are hypercellular areas with increased vascularity. The hypercellular areas are not associated with pleomorphism, necrosis or any mitotic activity. Cellular myxomas do not progress to higher grade lesion and they do not metastasize. There is recurrence in 5-10% cases unless excised with a clear margin. Pathology report should comment on the following: - Microscopic location - (subcutaneous, intramuscular, intermuscular, juxtaarticular) - Margin - (circumscribed or infiltrative ) ; - Degree of cellularity ; - Degree of vascularity ; - Presence of any pleomorphism or mitotic activity ; - Presence or absence of cyst formation ; - Myxoid content ; - Collagen content ; - Presence or absence of muscle atrophy and edema. Differential diagnosis: Myxoid liposarcoma ; Myxofibrosarcoma; Low grade fibromyxoid sarcoma ; Myxoid neurofibroma and low-grade malignant peripheral nerve sheath tumour. (Classically intramuscular myxoma is hypocellular, hypovascular, shows no evidence of pleomorphism or mitotic activity and the cells are S100 protein negative. Vimentin is usually positive and rarely some cells may be actin positive.) Juxta-articular myxoma histologically resembles intramuscular myxoma but develops adjacent to large joints and involves periarticular ligaments, tendons, joint capsules and muscles. Almost 30% cases recur locally.
|