|

Custom Search
|
|
Dermpath-India Pathology of Glomus Tumour Dr Sampurna Roy MD 2022
|
 |
|
The glomus tumour is a
distinctive neoplasm which arises from modified smooth muscle cells of the
normal glomus body. The 2013 WHO classification of soft tissue
tumours includes glomus tumors, myopericytoma, myofibroma and
angioleiomyoma as members of the pericytic family of neoplasms. [ The glomus body is a specialized form of arteriovenous anastomosis which is involved in temperature regulation. There is a central coiled canal known as Suquet-Hoyer canal which is lined by plump endothelial cells. This is surrounded by longitudinal and
circular muscle fibres containing rounded epithelial appearing glomus
cells. ] Rarely, the tumour may occur in the gastrointestinal tract (stomach, small intestine, colon), trachea, lungs, mesentery, bone, vagina and the cervix. A glomus tumour is rare in the sinonasal region. Almost all cases of sinonasal glomus tumor are benign and are usually cured by complete excision. Cutaneous lesion usually occurs in adults (20- 40 years) and presents as small blue red nodule in the deep dermis or subcutis. Intravascular spread of the glomus tumour is rare and has been described in the stomach and subcutaneous tissue. Most frequent location is the forearm. The pathologist must be aware of this variant of glomus tumour to avoid misdiagnosis and unnecessary additional treatments. Glomus tumour proper (solid
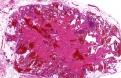
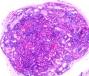
glomus tumour): Microscopic features: Histologically, this is a well circumscribed lesion characterized by solid aggregates of glomus cells around small capillary sized vessels in a myxoid or hyalinized stroma. The glomus cell is round, regular shaped with a sharply punched out rounded nucleus. Rare variants: I. Epithelioid: Unlike conventional glomus tumors, which consist of small polygonal cells with dark round nuclei and scanty cytoplasm, the epithelioid lesions are composed of large polygonal to spindle-shaped cells with abundant eosinophilic cytoplasm and large, irregularly shaped nuclei. The cells have both epithelioid and myoid qualities. Differential diagnosis: Spindle-cell lesions, such as schwannoma , leiomyoma, hemangiopericytoma.
II. Oncocytic: Three different clinical variants of glomangioma have been recognized: solitary, multiple, and nodular, or plaquelike. Glomangiomas are usually painless. These are mostly noted in adolescence and is less common than glomus tumour proper. Microscopic features: Histologically, these are poorly circumscribed, unencapsulated lesions characterized by prominent ectatic vessels and less conspicuous glomus cells. Secondary thrombosis and phlebolith formation may occur.
The features resemble those
of cavernous hemangioma. Overall features are similar to glomus tumour and glomangioma. There is gradual transition from round glomus cells to elongated smooth muscle cells. These features are more obvious near large blood vessels. Atypical and Malignant Glomus Tumour: I Classification of unusual glomus tumours: (Gould et al) 1. Locally infiltrative glomus tumour; 2. Cytologically malignant tumour arising and merging with typical glomus tumour (glomangiosarcoma arising in a benign glomus tumour). 3. De novo glomagiosarcoma Microscopic features: Histologically, the features are those of benign glomus tumour with sarcomatous areas consisting of short spindle cells with hyperchromatic nucleus (round cell or leiomyosarcomatous appearance) and prominent mitotic figures. II Classification of atypical glomus tumours: (Folpe et al.) 1. Malignant ; 2. Symplastic ; 3. Glomus tumors of uncertain malignant potential, and 4. Glomangiomatosis Atypical glomus tumour: Glomus tumours display unusual features, such as large size, deep location, infiltrative growth, mitotic activity, nuclear pleomorphism, and necrosis. Atypical features are usually observed centrally with a rim of benign-appearing glomus tumour. Malignant glomus tumour: Tumour with a deep location and a size of more than 2 cm, or atypical mitotic figures, or moderate to high nuclear grade and 5 mitotic figures or more/50 HPF. High nuclear grade alone, infiltrative growth, and vascular space involvement are not associated with metastasis.
Symplastic: High
nuclear grade in the absence other malignant features. Glomangiomatosis: Tumours with histologic features of diffuse angiomatosis and excess glomus cells. Immunohistochemistry: The tumour cells reveal
immunopositivity for vimentin, smooth muscle actin and muscle specific
actin in the cytoplasm. The cells do not stain with endothelial markers.
Desmin is occasionally only focally positive. Adnexal tumour- Eccrine spiradenoma (two population of cells and focal ductal differentiation); Hemangiopericytoma (spindle shaped cells and branching staghorn vessels); Intradermal naevus with pseudovascular spaces (focal nesting, S100 positive and evidence of maturation) ; Rhabdomyosarcoma; Ewing's sarcoma/PNET ; Hidradenoma ; Leiomyosarcoma with epithelioid change.
Note: Recent molecular studies have identified microRNA 143-NOTCH fusions or NOTCH1-3 rearrangements in benign and malignant glomus tumors. Novel MIR143-NOTCH fusions in benign and malignant glomus tumors. Genes Chromosomes Cancer. 2013;52:1075–87. Dermatopathology Quiz Case 144
|
|
|
 |