|

Custom Search
|
|
Infectious Disease Online Pathology of Smallpox Virus Infection (Variola Virus)
|
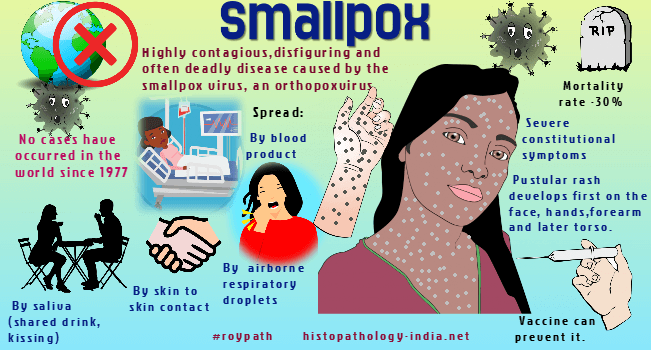
Before its eradication, smallpox (variola) was an acute, highly contagious, exanthematous viral infection.The virus contains a double-stranded DNA and produces a typical plaque, or "pock", when cultured on chorioallantoic membrane of embryonated chicken eggs. Visit: Chickenpox ; Since Jenner’s pioneering work in 1796, a similar virus - vaccinia, the causative agent of cowpox - has been used for "vaccination" to protect against small pox. Smallpox was evidently an ancient disease; a rash resembling smallpox was found in the mummified remains of the Egyptian Pharaoh Ramses V, who died in 1160 BC. The disease once had worldwide distribution in both urban and rural areas, afflicting persons of both genders and all ages, but particularly children. In 1967, the World Health Organization began its uniquely successful campaign to eradicate smallpox. By then, smallpox had already been controlled in most developed countries but was still endemic in the less developed world. In 10 years the vaccination campaign eradicated the disease. The successful eradication of smallpox depends on several factors, including the permanence of immunity following vaccination, the stability of the smallpox virus (in contrast to the genetic instability of influenza viruses and many others), and the lack of an animal reservoir for the virus. Smallpox was transmitted in respiratory droplets and almost always involved face to face contact. The virus infected the oropharynx or nasopharynx, multiplied in lymphoid tissue of the upper respiratory tract for about 2 day period of viremia and then entered a 4 to 14 day "latent" period, when it was undetectable in the blood and was assumed to be multiplying in the reticuloendothelial system. After another 1 or 2 day period of viremia, there was a 2 to 4 day prodrome of nonspecific febrile symptoms. The prodrome was followed by characteristic eruption of smallpox, which evolved through several stages, beginning as macules, then progressing over a 1 to 2 week period through papules, vesicles, and pustules. The pustules umbilicated within 2 weeks, and desiccated ("crust") to form scabs. The scabs, which contained the smallpox virus, usually sloughed from the skin, thereby creating fresh, pitted scars. Pitting or pockmarking was most common over facial areas that have numerous sebaceous glands. In the most severe form, black, "hemorrhagic small pox", which was almost always fatal, there was bleeding into the vesicles and pustules. Histologic features of the earliest stage of the rash included hyperemia, swelling of capillary endothelium, and perivascular infiltrates of lymphocytes and histiocytes in the upper dermis. Multiloculated vesicles developed by rupture of the membranes between degenerating epithelial cells. There was ballooning of cells in the lower levels of the stratum spinosum, and some degenerating cells fused into giant cells with two or more nuclei. Eosinophilic intracytoplasmic inclusion bodies (Guarnieri’s bodies) were prominent in ballooned epithelial cells. Secondary bacterial infections during the pustular stage led to complications such as keratitis, laryngitis, bronchitis, bronchopneumonia, encephalitis, osteomyelitis, and orchitis. Viral keratitis and secondary bacterial infections of the eyes were frequent complications. Many patients in Asia developed corneal ulcerations, and smallpox was usually the primary cause of blindness during epidemic periods. In pregnant women, the disease frequently caused abortion. |
|
Smallpox
vaccination in the preoutbreak setting is contraindicated for
persons who have the following conditions or have a close contact
with the following conditions:
1) A history of atopic dermatitis (commonly referred to as eczema), irrespective of disease severity or activity; 2) Active acute, chronic, or exfoliative skin conditions that disrupt the epidermis; 3) Pregnant women or women who desire to become pregnant in the 28 days after vaccination; and 4) Persons who are immunocompromised as a result of human immunodeficiency virus or acquired immunodeficiency syndrome, autoimmune conditions, cancer, radiation treatment, immunosuppressive medications, or other immunodeficiencies. Additional contraindications that apply only to vaccination candidates but do not include their close contacts are persons with smallpox vaccine-component allergies, women who are breastfeeding, those taking topical ocular steroid medications, those with moderate-to-severe intercurrent illness, and persons aged < 18 years. In addition, history of Darier disease is a contraindication in a potential vaccinee and a contraindication if a household contact has active disease.
|
|
|

